
Food allergy symptoms in adults: What you need to know and do
One minute you're enjoying your favorite shrimp scampi, and the next, you're dealing with hives and an upset stomach. What gives?
Food allergy symptoms in adults can pop up seemingly out of nowhere, ranging from annoying skin rashes and digestive issues to terrifying, life-threatening reactions. These symptoms usually hit fast—within minutes to a couple of hours after eating—and can affect your skin, gut, or even your breathing.
Why Adults Suddenly Develop Food Allergies
It’s a huge myth that food allergies are just a childhood problem. The truth is, your immune system can change its mind at any point, suddenly flagging a food you've eaten for years as a dangerous intruder. This is called adult-onset food allergy, and it can be incredibly confusing and scary when a go-to meal becomes an overnight threat.
This guide will break it all down for you. We’ll cover the full spectrum of symptoms, explain the crucial difference between a true allergy and a food intolerance, and walk you through the exact steps for getting diagnosed and managing your health safely.
A Growing Reality for Adults
If this is happening to you, you're not alone. Millions of adults are learning to navigate new dietary landmines. As of 2021, about 16 million adults in the United States—that's 6.2% of the adult population—are living with food allergies.
Interestingly, there's a noticeable gender gap: 7.8% of women report food allergies, compared to just 4.6% of men. You can dig into more of these food allergy statistics to see the bigger picture.
When you're trying to figure out what's going on, it's also smart to look at the connection between what you eat and how your skin reacts. Understanding how diet affects skin redness can give you clues about potential triggers that show up on your skin.
Think of your immune system as a bouncer at a club. For years, it's recognized shrimp as a regular and lets it right in. Then one day, maybe after an illness, stress, or hormonal shifts, the bouncer gets new orders. Suddenly, shrimp is on the "do not admit" list. The bouncer sounds the alarm, and that's when you get an allergic reaction.
Recognizing the Full Spectrum of a Food Allergy
When your immune system mistakenly flags a food as a dangerous invader, it launches a full-scale chemical counterattack. The results are the food allergy symptoms in adults you see and feel, which can pop up in different parts of your body, sometimes all at once.
Think of it like a faulty fire alarm system. Sometimes, a little smoke just sets off one detector. Other times, it triggers every alarm in the building.
Reactions usually show up fast—anywhere from a few minutes to two hours after eating. Knowing what to look for is your first line of defense. Let's break down the common signs by body system so you can connect the dots when a reaction starts.
Common Food Allergy Symptoms in Adults by Body System
To make it easier to spot a potential reaction, here’s a quick rundown of what you might experience and where.
| Affected System | Common Symptoms | Typical Onset Time |
|---|---|---|
| Skin | Hives, eczema flare-ups, swelling (lips, face, tongue), itching, tingling | Minutes to 1 hour |
| Gastrointestinal | Abdominal cramps, nausea, vomiting, diarrhea | 30 minutes to 2 hours |
| Respiratory | Wheezing, shortness of breath, tight throat, trouble swallowing, runny nose, congestion | Minutes to 1 hour |
| Cardiovascular | Dizziness, lightheadedness, fainting, weak pulse, pale or blue skin | Can be rapid; often part of a severe reaction |
This table is a great starting point, but remember that reactions can be unpredictable. You might have a skin reaction one time and a gut reaction the next, even from the same food.
Skin Reactions: The First Warning Signs
More often than not, your skin is the first to send up a red flag. These visible, and often incredibly uncomfortable, symptoms are caused by the release of chemicals like histamine, which brings on inflammation and irritation.
You might see or feel:
- Hives (Urticaria): Itchy, raised red or white welts that can appear out of nowhere and even seem to move around your body.
- Eczema (Atopic Dermatitis): If you already have eczema, a food allergen can trigger a major flare-up, causing those familiar red, scaly, and intensely itchy patches.
- Swelling (Angioedema): This is deeper swelling under the skin, most often affecting the lips, tongue, eyelids, or even the whole face.
- Itching or Tingling: This can be one of the very first clues. An itchy mouth or throat right after eating is a classic early sign of an allergic reaction.
Gastrointestinal Distress: When Your Gut Rebels
Once the problem food makes its way into your digestive system, your body’s defense mechanisms kick into high gear. The goal is to get the "threat" out, and that process can cause some serious discomfort.
Look for gut-related symptoms like:
- Abdominal Pain: This isn't just a mild stomachache; it's often sharp, cramping pain.
- Nausea and Vomiting: Your body might try to forcefully eject the allergen.
- Diarrhea: This is another common way your gut tries to quickly clear the offending food from your system.
While these symptoms can be confused with a simple food intolerance, an allergic reaction involves your immune system and often comes paired with other signs, like hives. It's a system-wide alert, not just a digestive issue.
These reactions are more common than you might think. For instance, eczema affected 7.3% of U.S. adults in 2021, and food allergies are a known trigger. A whopping 90% of these reactions are caused by just nine foods: milk, eggs, peanuts, tree nuts, fish, shellfish, wheat, soy, and sesame. You can read the full research about these allergy statistics for a deeper dive.
Respiratory and Cardiovascular Symptoms: When It Gets Serious
This is where a food allergy can shift from uncomfortable to dangerous. When a reaction affects your breathing or your heart, it's a clear sign that things are escalating. These symptoms demand immediate attention.
The progression from a simple skin rash to breathing difficulties is like a small kitchen fire suddenly engulfing the entire house. It means the reaction is spreading fast and becoming a true emergency.
Keep an eye out for these respiratory and cardiovascular red flags:
- Wheezing or Shortness of Breath: If your airways start to constrict, you might hear a whistling sound when you breathe or feel like you can't get enough air.
- Trouble Swallowing or a Tight Throat: Swelling in the throat can make it feel tight or like there's a lump, which is a very serious warning sign.
- Nasal Congestion or a Runny Nose: Just like seasonal allergies, your nasal passages can become inflamed and stuffy.
- Dizziness or Fainting: This is a sign of a drop in blood pressure. Feeling lightheaded or actually passing out means the reaction is severe.
- Pale or Blue-Tinged Skin: A change in skin color indicates poor circulation and is a hallmark of anaphylaxis, the most severe type of allergic reaction.
Understanding the full spectrum of food allergy symptoms in adults is critical. What starts as an itchy mouth could be the first step toward a severe, multi-system reaction. By knowing these signs, you can react faster and get the right help the moment your body sounds the alarm.
Allergy vs. Intolerance: What's Really Going On?
When a certain food makes you feel unwell, it’s natural to wonder if you have an allergy. But not every bad reaction is a true allergic one. Getting to the bottom of it means understanding a critical difference: is your immune system sounding a false alarm, or is your digestive system just having a bad day?
Knowing the distinction between a food allergy and a food intolerance is the first, and most important, step toward managing your symptoms and feeling better. It all comes down to how your body is actually responding.
Think of a food allergy as your body's security system going haywire. It mistakes a harmless food protein for a dangerous invader and launches a full-scale, body-wide emergency response. On the other hand, a food intolerance is more like a traffic jam in your gut—it's frustrating, causes some local chaos, but doesn't trigger a system-wide meltdown.
This core difference is why the symptoms, severity, and treatment for each are worlds apart.
The Immune System's Overreaction
A true food allergy is your immune system getting it wrong. The first time you eat an offending food, your body produces specific antibodies called Immunoglobulin E (IgE). These IgE antibodies then arm certain immune cells, priming them for the next encounter.
The next time that food enters your system, the IgE antibodies spot it immediately. They signal those armed cells to release a flood of chemicals, most notably histamine. This chemical cascade is what causes the classic food allergy symptoms in adults, ranging from annoying hives to life-threatening anaphylaxis.
Because this is a full-body immune response, the symptoms can pop up almost anywhere:
- Skin: Hives, relentless itching, or swelling of the lips and face.
- Respiratory System: Wheezing, sudden shortness of breath, or a terrifying tightening in your throat.
- Gastrointestinal Tract: Abdominal cramps, vomiting, or diarrhea.
- Cardiovascular System: Dizziness, a sharp drop in blood pressure, or even fainting.
These reactions can strike fast, be incredibly severe, and are potentially fatal. That's why allergies demand serious respect—even a microscopic amount of the food can trigger a major event.
When It’s Just a Digestive Issue
A food intolerance, meanwhile, almost never involves your immune system. It’s usually a simple mechanical problem within your digestive tract. Your body might not be making enough of a specific enzyme needed to break down a food, leading to symptoms that are uncomfortable but not dangerous.
The most well-known example is lactose intolerance. People with this condition don't produce enough lactase, the enzyme required to digest milk sugar. The undigested sugar then ferments in the gut, causing that familiar gas, bloating, and diarrhea—a digestive traffic jam, not an immune system attack.
Symptoms of an intolerance are typically confined to the gut and are often dose-dependent. A small bite might cause no trouble at all, while a full serving leads to an evening of discomfort.
For a deeper dive into this crucial topic, check out our complete guide explaining the difference between food intolerance and allergy. Nailing down this distinction is fundamental to your health journey. While intolerances are a nuisance, true allergies are a serious medical condition that require a completely different approach to management and care.
How To Get a Definitive Diagnosis
If you think a certain food is causing your symptoms, the next step is getting a real answer. Guessing isn't a strategy when it comes to potential food allergy symptoms in adults, because a future reaction could be much worse than the last. The path to a diagnosis is a careful investigation, blending your own observations with medical testing to find the truth.
This whole process doesn't start in a clinic—it starts at your kitchen table. Before any tests are run, the single most powerful first step you can take is to become a detective of your own diet.
Start with a Detailed Food and Symptom Diary
Your allergist’s most valuable tool is the information you bring to them. Keeping a detailed food and symptom diary for a couple of weeks creates a clear roadmap for diagnosis. Think of it as gathering evidence—the more detailed your notes are, the easier it is for your doctor to spot the likely culprit.
For every meal, snack, and drink, make sure you log:
- What you ate: Be specific. Instead of "sandwich," write "turkey, cheddar cheese, and mayo on whole wheat bread."
- When you ate it: Note the exact time.
- What symptoms appeared: List everything you felt, from an itchy mouth or hives to stomach cramps or dizziness.
- When symptoms started: How long after eating did the reaction kick in? Was it minutes or hours later?
This log helps connect the dots between a specific food and a reaction, narrowing down the list of suspects before you even set foot in a clinic.
Professional Allergy Testing Methods
Once you have your diary in hand, it’s time to see a medical professional for formal testing. An allergist will use your notes to decide which tests make the most sense for you. The goal is to confirm the presence of Immunoglobulin E (IgE) antibodies, which are the specific immune proteins that trigger true allergic reactions.
The two most common ways to do this are skin-prick tests and blood tests. For a deeper look at how they stack up, you can learn more about the differences in an allergy blood test vs skin test to see which might be better for your situation. Both are excellent tools for spotting the IgE antibodies linked to food allergens.
An IgE test is like a security check for your immune system. It reveals which foods your body has mistakenly flagged as dangerous, giving you and your doctor a clear list of what to avoid.
Before we dive into the specifics of each test, here’s a quick overview of the most common diagnostic methods.
Comparing Food Allergy Diagnostic Methods
| Diagnostic Method | How It Works | Pros | Cons |
|---|---|---|---|
| Skin-Prick Test | A tiny amount of liquid allergen is pricked into the skin's surface. A raised bump (wheal) indicates a positive reaction. | Fast results (15-20 mins), highly sensitive, cost-effective. | Can't be done if you have severe eczema or take certain medications (like antihistamines). |
| Blood Test (IgE) | A blood sample is taken and sent to a lab to measure the amount of specific IgE antibodies to various foods. | One needle poke can test for many allergens; unaffected by medications. | Slower results (days to a week); can sometimes show false positives. |
| Oral Food Challenge | You eat small, gradually increasing amounts of the suspected allergen under strict medical supervision. | The "gold standard" for a definitive yes/no answer; highly accurate. | Time-consuming; carries a risk of a severe reaction (must be done in a clinical setting). |
| Food Diary & Elimination Diet | You meticulously track what you eat and your symptoms, then remove suspected foods to see if symptoms improve. | No cost; empowers you to identify triggers yourself. | Requires commitment and can be difficult to interpret without a professional's guidance. |
Each of these methods provides a different piece of the puzzle. An allergist will help you decide which combination of tests is the right approach for getting a clear and reliable diagnosis.
Convenient At-Home Screening Options
For those who want a convenient and private place to start, at-home testing can offer valuable initial insights. The Barb N.P. At-Home Allergy Test Kits provide a straightforward way to screen for a wide array of common food allergens from a simple sample, all from the comfort of your home.
These panels deliver comprehensive results that you can then discuss with your healthcare provider. This approach empowers you to have a more informed, productive conversation, potentially fast-tracking your path to a solid diagnosis and management plan.
The Gold Standard: The Oral Food Challenge
Sometimes, skin and blood tests just don't give a conclusive answer. In these situations, an allergist might recommend an oral food challenge. This is considered the absolute gold standard for diagnosing a food allergy because it directly observes your body's reaction to the food in real-time.
During the test, you'll eat small, gradually increasing amounts of the potential allergen in a clinical setting, under strict medical supervision. The medical staff watches you closely and is ready to treat any reaction immediately. Because of the risk, this test should never be tried at home. It's the most accurate way to confirm or rule out an allergy, providing a definitive yes or no answer.
Responding to Anaphylaxis: The Most Severe Reaction
While most food allergy symptoms are manageable, some can escalate into a frightening, life-threatening crisis called anaphylaxis. This is the most severe allergic reaction you can have, and it demands immediate, clear-headed action. When anaphylaxis hits, every second counts.
Think of it as your immune system’s alarm bells ringing out of control. Instead of a localized reaction like a few hives, the chemicals flood your entire body at once. This triggers a dangerous chain reaction: blood vessels widen, blood pressure plummets, and airways can swell shut, making it terrifyingly difficult to breathe.
Recognizing the Warning Signs of Anaphylaxis
Anaphylaxis can explode out of nowhere, often within minutes of eating the trigger food. The symptoms can hit multiple parts of the body simultaneously, creating an overwhelming and scary situation. Knowing what to look for is the first step in saving a life.
Key warning signs include:
- Difficulty Breathing: This isn't just a stuffy nose. It can feel like wheezing, gasping for air, or the terrifying sensation that your throat is closing.
- Swelling: Look for noticeable swelling of the tongue, lips, or throat. This is a major red flag.
- Circulation Issues: A sudden drop in blood pressure can cause dizziness, a weak and rapid pulse, pale or blueish skin, and even fainting.
- Gastrointestinal Distress: Severe stomach pain, intense vomiting, or diarrhea can happen alongside other symptoms.
- A Sense of Impending Doom: This one sounds strange, but it's real. Many people report a sudden, overwhelming wave of anxiety or a feeling that something is terribly wrong.
This isn’t a rare occurrence. Globally, food allergies affect around 6-10% of adults. In the U.S. alone, 2021 data from the CDC shows that 6.2% of adults—that’s roughly 16 million people—have a diagnosed food allergy. Shellfish is one of the top triggers for these severe reactions. You can find more details in these important food allergy statistics on acaai.org.
If you're just starting to suspect you have a food allergy, this chart visualizes the path from your initial concerns to getting professional help.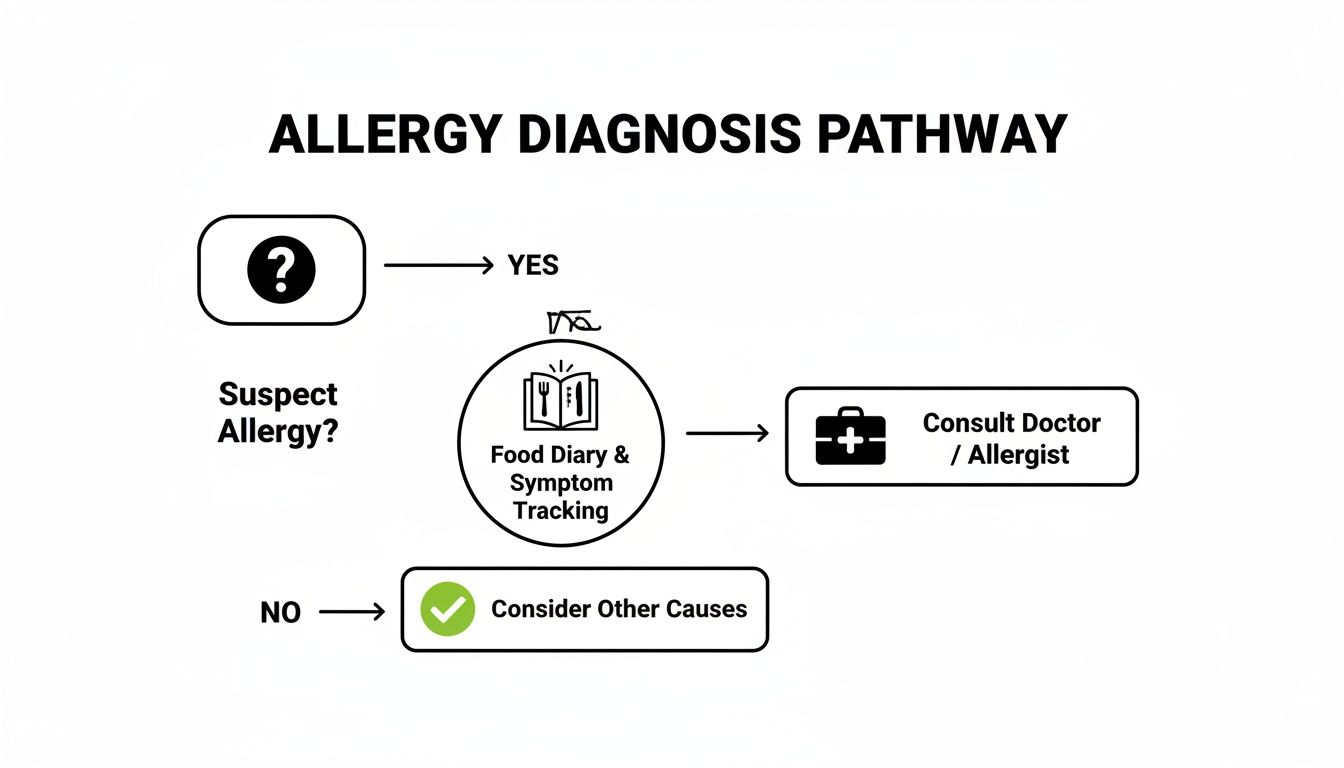
As you can see, the journey to a real diagnosis often starts with you—noticing patterns, maybe keeping a food diary—before you ever step into a doctor's office.
The Immediate Emergency Response Protocol
If you think someone is having an anaphylactic reaction, there is a clear, two-step plan. Do not hesitate. Do not wait and see.
In an anaphylactic emergency, epinephrine is the only first-line treatment. It’s not just helpful; it’s essential. It works instantly to reverse the life-threatening symptoms—constricting blood vessels to bring blood pressure back up, relaxing airway muscles to make breathing easier, and reducing dangerous swelling.
Here’s exactly what to do:
- Administer Epinephrine Immediately: Use an epinephrine auto-injector (like an EpiPen) at the very first sign of a severe reaction. Give the injection into the outer thigh. Don’t wait for symptoms to get worse.
- Call for Emergency Medical Help: Dial 911 (or your local emergency number) immediately and tell them someone is having an anaphylactic reaction. Even if the person feels better after the shot, they still need to go to the hospital. A second, delayed wave of symptoms (called biphasic anaphylaxis) can occur hours later.
Anaphylaxis always requires a trip to the emergency room. Never assume the danger has passed just because the initial symptoms have calmed down. Knowing these steps empowers you to act with confidence in a crisis, turning a potentially tragic moment into a manageable one.
Daily Management and Skin Health Strategies
Living with a food allergy means you have to become more mindful, but it doesn't have to shrink your world. It's really about mastering a few key skills—like reading labels like a detective and learning how to speak up for yourself—so you can navigate daily life with confidence.
Managing food allergy symptoms in adults comes down to vigilance, especially when you're not in your own kitchen. The CDC has reported that about half of all fatal allergic reactions happen because of restaurant food. That statistic really underscores how critical it is to communicate clearly and choose carefully when dining out.
Mastering Everyday Life with a Food Allergy
Your daily routine might need a few tweaks, but it doesn’t have to feel restrictive. The goal is to build a toolkit of simple habits that eventually become second nature.
Here are the non-negotiables:
- Become a Label Expert: Food labels are your best friend. Always read the entire ingredient list, even on products you buy all the time, because companies can change their formulas without any fanfare. Look for the "contains" statements and pay close attention to any "may contain" warnings about cross-contamination.
- Communicate Clearly When Dining Out: Never, ever assume a dish is safe. When you're at a restaurant, tell your server about your allergy right away. Ask specific questions about how things are prepared—don't be shy about asking to speak with the chef if you need extra reassurance.
- Plan Ahead for Social Events: Heading to a party? Eat a safe meal before you go. That way, you won't be starving and tempted by food you can't verify. Another great tip is to bring a safe dish you can share, guaranteeing you'll have something delicious and worry-free to enjoy.
For anyone navigating a diagnosed allergy, knowing what's in your food is everything. This guide to the top 8 allergen-free snacks is a great resource for finding safe and tasty options.
The Connection Between Food Allergies and Skin Health
Food allergies are an inside job, but the evidence often shows up on your skin. When you have an allergic reaction, your body releases a flood of histamine and other inflammatory chemicals, and your skin is frequently the first place you'll see the fallout.
You might notice a few common things:
- Hives (Urticaria): Those sudden, maddeningly itchy, raised welts.
- Eczema (Atopic Dermatitis) Flare-ups: If you already have eczema, an allergen can make it dramatically worse.
- Angioedema: This is a deeper kind of swelling, usually around the eyes, lips, and face.
- General Redness and Inflammation: Sometimes, your skin just becomes flushed, sensitive, and irritated all over.
All this inflammation can weaken your skin's natural protective barrier, leaving it more vulnerable and reactive than usual. If you're dealing with the aftermath of a reaction, learning how to repair a damaged skin barrier gives you a clear, actionable game plan for recovery.
Think of your skin as a window to your immune system's activity. When an allergen triggers an internal alarm, that inflammation often becomes visible on the surface, signaling that your body is in defense mode.
Soothe Your Skin with Advanced Self-Care
Calming your skin down after a reaction is a huge part of managing the visible side of a food allergy. While avoiding your triggers is always goal number one, having the right tools to help your skin heal can make a world of difference in your comfort and confidence.
This is where targeted, at-home treatments can be a game-changer. One of the most effective and gentle options is LED light therapy.

The Barb N.P. LED Facial Mask, for example, is designed to bring professional-level skin support right into your living room. It’s completely wireless, so you can actually relax while using it, and it fits comfortably on your face.
The mask offers three distinct lighting settings, but for allergy-related skin issues, the red light is the star. It's known to help reduce inflammation and promote healing. By making this part of your self-care routine, you can actively soothe redness and irritation, helping your skin bounce back faster after an inflammatory event. It’s a simple, powerful way to manage the external symptoms and get your skin back to a calm, balanced state.
Your Top Questions About Adult Food Allergies, Answered
When you're navigating the confusing world of adult-onset allergies, questions and misinformation can pop up everywhere. Let's clear the air and get you some direct, expert-backed answers on food allergy symptoms in adults.
Can I Really Develop an Allergy to Something I've Eaten My Whole Life?
Believe it or not, yes. It’s called an adult-onset allergy, and it’s more common than you might think. Your body isn't static; changes in your immune system, environment, or even hormones can suddenly make it see a familiar food protein as a threat, sparking a brand-new allergic reaction.
What Are the Most Common Food Culprits for Adults?
The allergy landscape definitely shifts as we get older. While kids often deal with milk and egg allergies, for adults, the big ones are shellfish (think shrimp and lobster), followed by peanuts, tree nuts (like walnuts and almonds), and fish. Allergies to soy, wheat, and sesame are also frequently seen in the adult population.
Is a Mild Rash Really a Big Deal? Should I See a Doctor?
Absolutely, one hundred percent. Even if a symptom seems minor—a few hives, a little itch—getting a professional diagnosis is non-negotiable. The next time you encounter that food, the reaction could be dramatically more severe and even escalate to life-threatening anaphylaxis.
A proper diagnosis from a clinician is the only way to confirm the allergy, get a prescription for an emergency epinephrine auto-injector, and create a management plan to keep you safe. Don't risk it.
Can Stress Make My Food Allergies Worse?
It sure can. While stress doesn't cause a food allergy to develop, it can absolutely pour fuel on the fire. When you're stressed, your body's inflammatory response is heightened, which can turn what might have been a mild reaction into something much more serious. Managing your stress is a crucial part of holistic allergy care.
At BotoxBarb, we know that true wellness means caring for your health from the inside out. Whether you need diagnostic insights or advanced skincare solutions to manage external symptoms, our mission is to empower you on your health journey. Explore our curated collection of medical-grade products and book an expert consultation today at https://barbnp.shop.


