
How to Read Allergy Test: A Clear Guide on how to read allergy test
So, you have your allergy test results in hand. Staring at that page full of medical terms, numbers, and abbreviations can feel like trying to crack a code. But don't worry, it's simpler than it looks.
The key to reading your allergy test is knowing which metric to focus on. For a skin prick test, you'll look at the wheal size in millimeters (mm). For a blood test, it's all about the specific IgE levels, measured in kilounits per liter (kU/L). In both cases, a bigger number generally points to a stronger sensitization to that allergen.
Your Guide to Understanding Allergy Test Results

Whether the report landed in your email or was handed to you by your doctor, it represents the first big step toward clarity. But faced with columns of unfamiliar names and data, it’s completely normal to feel a bit lost. This guide is here to translate that document into plain English, so you can finally understand the signals your body is sending.
We’ll start by breaking down the two most common types of allergy tests: the skin prick test (SPT) and the IgE blood test. Each one measures your body's reaction to potential triggers in a different way, and knowing which test you had is the first piece of the puzzle.
The Foundation of Allergy Testing
At its core, any allergy test is designed to pinpoint the specific triggers that make your immune system overreact. When you’re exposed to an allergen—whether it's pollen, pet dander, or a certain food—your body can produce antibodies called Immunoglobulin E (IgE).
These IgE antibodies are the culprits that trigger the release of chemicals like histamine, leading to all those classic allergy symptoms: the sneezing, itching, hives, and swelling.
- Skin Prick Test (SPT): This test gives you visual, real-time feedback. An allergist introduces a tiny amount of a suspected allergen just under your skin's surface. A positive reaction shows up as a raised, itchy bump (called a "wheal") within about 15-20 minutes.
- IgE Blood Test: This lab test measures the amount of specific IgE antibodies circulating in your bloodstream. Higher levels of IgE linked to a particular substance suggest you're sensitized to it.
Understanding this difference is crucial because the way you interpret the numbers depends entirely on which test you’ve taken.
To quickly summarize, here are the core metrics you'll be looking at.
Quick Guide to Common Allergy Test Metrics
| Test Type | What It Measures | Common Units/Metrics |
|---|---|---|
| Skin Prick Test (SPT) | The size of the raised, itchy bump ("wheal") on the skin. | Millimeters (mm) |
| IgE Blood Test | The concentration of specific IgE antibodies in the blood. | Kilounits per liter (kU/L) or a Class Scale (e.g., 0-6) |
These are the primary numbers that tell the story of your potential sensitizations.
Why Accurate Interpretation Matters
Being able to read an allergy test properly is more important than ever. Allergies are on the rise globally, impacting nearly 40% of the world's population, with some estimates showing annual increases of 10-15%. Here in the US, the CDC tracked 32 million food allergy cases in 2022 alone. The numbers are staggering.
A test result is just one piece of the puzzle, not a final diagnosis. The most important step is to connect the numbers on the page with your real-life symptoms. A positive result for dust mites means a lot more if you wake up congested every single morning than if you have no symptoms at all.
For those just starting to investigate their symptoms, at-home allergy testing kits from BARB N.P. offer a great starting point. These kits provide a convenient way to gather initial data on potential food and environmental sensitivities from the comfort of home.
If you're curious about this option, you can learn more in our guide to allergy testing at home. Gathering this information first can empower you to have a much more productive conversation with a healthcare professional down the line.
Decoding Your Skin Prick Test Report

One of the biggest advantages of a skin prick test (SPT) is the immediate visual feedback. Forget waiting days for lab results—in about 20 minutes, you can literally see how your body responds to different allergens right on your arm.
But staring at a grid of red, itchy bumps can feel like trying to read a foreign language. Learning how to read an allergy test like this is all about knowing what to look for, starting with the controls. These are the baseline checks that ensure the test itself is accurate.
The Importance of Positive and Negative Controls
Think of the controls as the test's internal fact-checkers. Every single SPT panel includes two crucial benchmarks to confirm your results are valid and your skin is behaving as it should.
- The Positive Control (Histamine): A tiny drop of histamine is applied to your skin. Since histamine is the very chemical your body unleashes during an allergic reaction, everyone should get a small red bump here. This proves your skin is capable of showing a reaction.
- The Negative Control (Saline): A sterile saline solution (basically saltwater) is also applied. Your skin shouldn't react to this at all. This check ensures your skin isn't just hyper-sensitive and reacting to the prick itself, which would give you a slate of false positives.
Bottom line: If you don't react to the histamine or you do react to the saline, the entire test is considered unreliable. It’s the first thing any practitioner looks at.
Interpreting the Wheal and Flare
Once you know the controls are good, you can move on to the interesting part—the allergen results. An allergic reaction on the skin has two components: the "wheal" and the "flare."
The wheal is the raised, pale bump that looks a lot like a mosquito bite. This is the single most important measurement for a diagnosis. The flare is the flat, red area that spreads out around the wheal. While it's noted, its size isn't nearly as important as the wheal's.
An allergist measures the diameter of the wheal in millimeters (mm). Generally, a wheal that is 3mm or larger than the negative control is considered a positive result. This indicates you are "sensitized" to that allergen.
But size definitely matters here. A bigger wheal often points to a stronger level of sensitization. Let's look at a quick example.
Imagine your report shows the following:
- Dust Mites: 5mm wheal
- Timothy Grass Pollen: 3mm wheal
- Cat Dander: 8mm wheal
This readout suggests a very strong sensitization to cat dander, a moderate one to dust mites, and a low-level one to Timothy grass. For many, skin reactions from allergies can cause persistent irritation and redness. Managing this inflammation is a key part of feeling better.
If skin health is a concern, products like the Barb N.P. LED Facial Mask can be a great addition to your routine. It's wireless and designed for comfort, so you can easily wear it while relaxing. The mask features three distinct lighting settings to target different skin concerns, helping to calm inflammation and support overall skin wellness.
Why Your Symptoms Are the Final Piece of the Puzzle
This is the most critical takeaway: a positive skin test only confirms sensitization, not a true clinical allergy. All it means is that your body produces IgE antibodies against that substance. It doesn't guarantee you'll actually have symptoms when you're exposed.
Your results have to be connected to your real-world experiences to mean anything.
For example, that 5mm wheal to dust mites is far more significant if you wake up every morning with a stuffy nose and sinus headache. Likewise, a 3mm wheal to pollen carries much more weight if you can't walk through a park in the spring without a sneezing fit.
The test results are just clues, not the final verdict. An experienced practitioner will always put these findings together with your detailed symptom history to build an accurate diagnosis. If you're exploring different testing methods, our article comparing allergy blood tests vs. skin tests is a great resource for understanding the pros and cons of each.
Making Sense of IgE Blood Test Results

While a skin prick test gives you those instant visual clues, an IgE blood test delivers its verdict in a detailed data report. At first glance, that sheet of numbers and acronyms can feel pretty intimidating. But learning how to read allergy test results from a blood draw is really just about getting familiar with a few key metrics.
The entire report boils down to one crucial thing: specific IgE (sIgE) antibodies. These are the unique immune proteins your body produces when it encounters a specific allergen. The test quantifies exactly how many of these antibodies are floating around for each substance tested, giving you a hard number for your body’s level of sensitization.
Understanding the Numbers: kU/L and Class Ratings
Your results will show up in a standard unit of measurement: kilounits of antibody per liter (kU/L). It’s simple—a higher kU/L value points to a bigger concentration of IgE antibodies, which in turn suggests a stronger sensitization to that specific allergen.
To make things even clearer, labs often group these numbers into a "Class" system, which usually goes from Class 0 up to Class 6. Think of it as a handy reference guide that translates the raw kU/L data into a much more digestible rating. For example, a Class 1 result flags a very low level of sensitization, while a Class 5 or 6 shows an extremely high level.
Figuring out these results isn't just an academic exercise—it's a game-changer for the millions dealing with allergic rhinitis and asthma. Globally, somewhere between 10-30% of people have allergic diseases, and it’s no surprise that in-vivo tests like skin pricks make up the bulk of the USD 3.5 billion allergy testing market in 2024.
Let's put it into a real-world context. Say you get an allergy panel from a clinic like BotoxBarb that includes both tests. A skin prick test might show a 4mm wheal for dust mites—that’s a positive reaction if the histamine control looks similar after 15-20 minutes. But for foods, skin tests can be less specific, so you need to connect the dots with your personal history. An itchy throat right after eating shrimp that lines up with an IgE Class 4 (17.50 - 49.99 kU/L) result points strongly to a true allergy. You can dive deeper into the clinical side of this with these allergy test interpretation guidelines.
IgE Antibody Levels and Allergy Classes Explained
This table breaks down the common IgE test result classes, their kU/L values, and what they generally mean for your level of sensitization.
| Class | IgE Level (kU/L) | Interpretation |
|---|---|---|
| Class 0 | < 0.35 | Negative or Undetectable |
| Class 1 | 0.35 - 0.69 | Very Low Level |
| Class 2 | 0.70 - 3.49 | Low Level |
| Class 3 | 3.50 - 17.49 | Moderate Level |
| Class 4 | 17.50 - 49.99 | High Level |
| Class 5 | 50.00 - 99.99 | Very High Level |
| Class 6 | > 100 | Extremely High Level |
With this table, you can start to contextualize your own results. A Class 2 for peanuts might mean you need to be cautious and definitely talk to your doctor. On the other hand, a Class 5 for birch pollen almost certainly confirms it's the main trigger for your seasonal misery.
The Real-World Meaning of High and Low Levels
It’s completely natural to see a high number on your report and feel a wave of panic. But it’s critical to understand what these levels really tell you—and what they don’t.
Just like with a skin prick test, a positive IgE blood test confirms sensitization, not necessarily a clinical allergy. A higher class number increases the probability of an allergic reaction, but it doesn't predict the severity of that reaction.
Someone with a Class 2 sensitization to milk could experience a severe anaphylactic reaction, while another person with a Class 5 might only get a few mild hives. The numbers are an incredibly powerful guide, but they are not a crystal ball.
For many people, allergic reactions show up on the skin as inflammation, redness, and general irritation. Calming that stressed skin is a huge part of feeling better. A fantastic tool for this is the Barb N.P. LED Facial Mask. It’s completely wireless and designed for comfort, making it easy to fit into your daily routine. It also features three distinct lighting settings that target different skin issues, from reducing redness to helping you achieve a clearer complexion.
Ultimately, your blood test results are a vital piece of the puzzle. The most important next step is to discuss them with a healthcare professional. They can place the numbers in the context of your specific symptoms and medical history to build a complete and accurate picture of your allergies.
Why a Positive Allergy Test Doesn't Always Mean You're Allergic
Have you ever gotten your allergy test results back, seen a positive mark next to something you eat all the time, and thought, "That can't be right"? It's an incredibly common reaction. Learning how to read an allergy test isn't just about looking at the positives and negatives; it's about understanding the story behind the numbers. Sometimes, your immune system gets its wires crossed.
The single most important concept here is the difference between being sensitized and having a true clinical allergy. A positive test—whether it’s a raised welt on your skin or a high number on a blood report—only proves sensitization. It means your body has created IgE antibodies against that substance. It does not automatically mean you'll break out in hives every time you're near it.
The Tricky Business of Cross-Reactivity
One of the biggest culprits behind these confusing results is a phenomenon called cross-reactivity. This happens when the proteins in one substance look so similar to the proteins in another that your immune system can't tell them apart. It spots one allergen it knows it dislikes and mistakenly flags the other one as a threat, too.
A perfect, real-world example is Oral Allergy Syndrome (OAS). Someone might have a raging allergy to birch pollen. Because the proteins in birch pollen are molecular look-alikes to proteins in certain raw fruits, nuts, and veggies, their body gets confused.
- The Test Says: Their report shows a very high IgE level for birch pollen.
- Their Life Says: They don't just get hay fever in the spring. They also get an itchy, tingly mouth whenever they bite into a raw apple, a piece of celery, or a handful of almonds.
In this case, they aren't truly allergic to apples. Their body is just cross-reacting due to the primary pollen allergy. The apple is an innocent bystander caught in the crossfire. Understanding this can save you from a lot of unnecessary and stressful dietary restrictions. You can dive deeper into the nuances of test results in our article on how accurate allergy tests are.
What a "False Positive" Really Means
This brings us to the idea of a false positive—the test says you're allergic, but you have zero symptoms when you're exposed. Skin prick tests, for instance, are fantastic at ruling allergies out. A negative result is highly reliable. But they are known to sometimes over-report allergies, leading to these head-scratching positive results.
The key to making sense of it all is connecting the dots between the data and your personal history. Sure, a Class 6 IgE result for shrimp seems scary, but if you've been eating shrimp cocktail your whole life without issue, your personal experience wins.
Skin tests are considered positive with a raised bump (wheal) of 3mm or more. They are about 90% sensitive for foods but only 50% specific, which is exactly why allergists don't recommend broad, random screening without a history of symptoms. It takes a trained eye to tell the difference between a true allergy and a false alarm from cross-reactivity.
A positive result without symptoms is just biological noise. Your allergy test results should always be used to confirm or rule out a suspicion you already have based on your own life experiences.
For many people, allergic reactions show up on the skin as persistent redness, inflammation, or irritation. Getting those symptoms under control is a huge part of feeling better. A fantastic tool for supporting calmer skin is the Barb N.P. LED Facial Mask. It’s thoughtfully designed to be wireless and comfortable, so it’s easy to use while you relax. It offers three distinct lighting settings to target different concerns, from reducing inflammation to promoting clearer-looking skin. Adding it to your routine can be a great step in managing the skin-related side effects of your sensitivities, helping you use your test results as a guide—not a set of rigid rules.
Turning Your Allergy Results Into an Action Plan
You've waded through the reports, decoded the numbers, and started connecting the dots to your symptoms. Now for the most important part: turning all that data into a practical plan that actually helps you feel better. Think of your results as a personalized roadmap, pointing you exactly where to focus your efforts.
This doesn't mean you need to overhaul your entire life overnight. A smart action plan starts with small, targeted changes based on your biggest triggers. The goal is simple: reduce your overall allergen load. When you do that, you give your immune system a chance to calm down, which can dramatically lessen your symptoms.
Connecting Results to Real-Life Changes
First, grab your test results and your symptom journal. Sit down and look for the most obvious connections—the high-ranking allergens that perfectly explain why you felt awful after that picnic or why you wake up congested. This is where you'll get the biggest bang for your buck.
From there, you can build a multi-pronged attack.
- Dietary Tweaks: If your report flagged food sensitivities, an elimination diet is your next logical step (always best done with a doctor's guidance). You'll remove a suspect food for a few weeks, then reintroduce it to see if symptoms flare up. It’s the gold standard for confirming a food trigger.
- Environmental Control: For culprits like dust mites, pollen, or pet dander, your home should be your sanctuary. This could mean investing in a good HEPA filter, zipping allergen-proof covers on your mattress and pillows, or washing your bedding in hot water every week.
- Symptom First-Aid: Keep your go-to over-the-counter antihistamines, decongestants, or nasal sprays ready for flare-ups. Knowing what gives you the fastest relief is a huge part of feeling in control.
As you start managing your triggers, you'll want to think about reducing exposure around the house. A great place to start is understanding What Type of Carpet Cleaning is Best for Allergies? to get rid of allergens hiding in your floors.
This decision tree shows exactly how to connect a positive test with your actual symptoms to figure out what to do next.
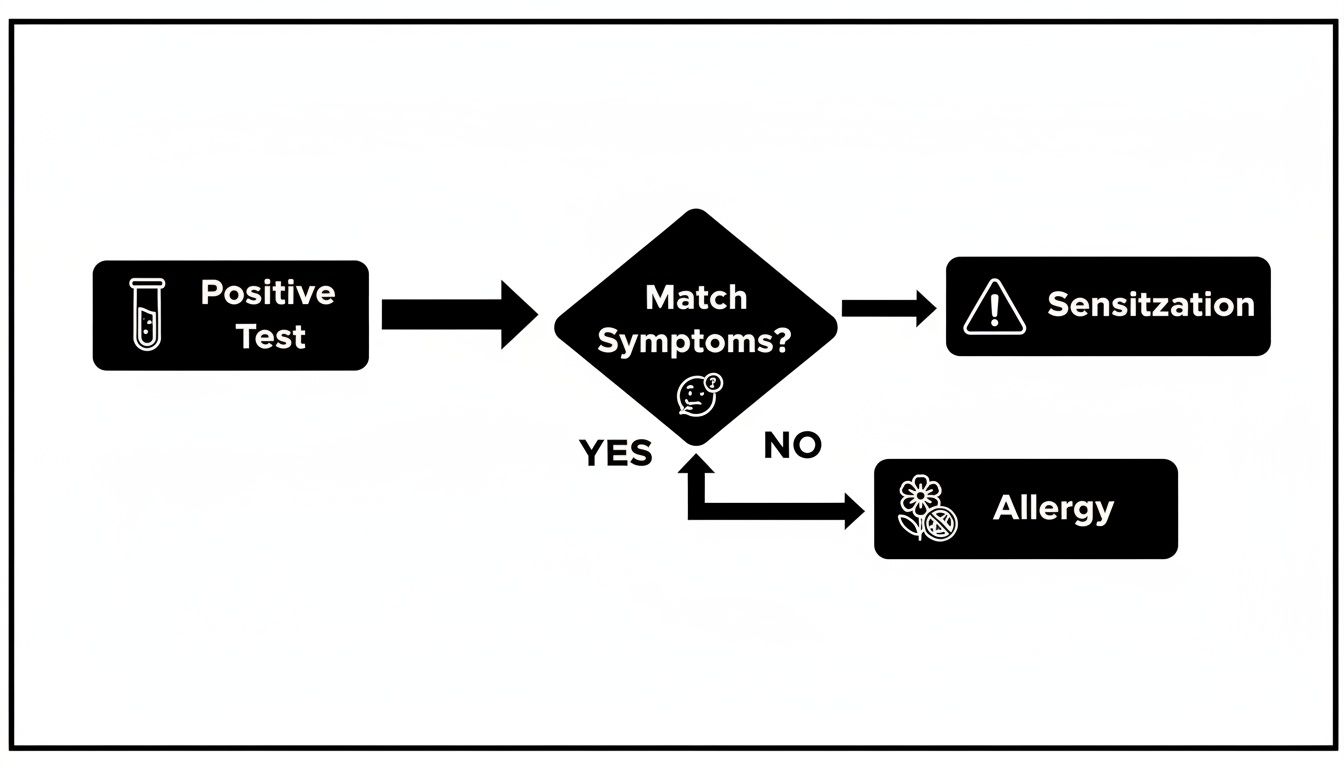
Remember, a positive test is just the first step. It's the presence (or absence) of symptoms that ultimately tells you whether you're dealing with a true allergy or just a sensitization.
Managing Allergy-Related Skin Issues
For many of us, allergic reactions show up right on our skin as redness, hives, or eczema flare-ups. Calming that external irritation is just as critical as managing your sniffles and sneezes. When your skin feels better, you feel better.
This is where targeted skincare tools can be a game-changer. The Barb N.P. LED Facial Mask is a fantastic addition to any skin-focused allergy plan. It's completely wireless and designed for comfort, so you can easily pop it on while you’re winding down for the night.
The mask has three different light settings, each with a specific job. You can use the red light to help calm inflammation, the blue light to target blemishes, or the amber light to work on evening out your skin tone. It’s a versatile way to customize your skincare based on what your skin needs that day.
Bringing a device like this into your routine helps you proactively tackle the visible side of your allergies, leading to calmer, healthier-looking skin. It’s a perfect example of using your test results to build a truly holistic wellness plan.
When to Call in a Specialist
While you can accomplish a lot on your own, sometimes you need to bring in a pro. Your test results are the perfect jumping-off point for a productive conversation with an allergist or immunologist.
You should definitely book an appointment if:
- Your symptoms are severe or messing with your daily life (think chronic sinus infections, persistent asthma, or intense skin reactions).
- You suspect a serious food allergy. An allergist can perform an oral food challenge, the only way to get a definitive diagnosis.
- Your results are confusing or contradictory. If you have a bunch of positives but can't figure out what's causing your symptoms, a specialist can help cut through the noise.
- You're ready for long-term treatment. An allergist can talk to you about options like immunotherapy (allergy shots or drops) that can actually desensitize your immune system over time.
A specialist can give you a final diagnosis and create a prescription-strength treatment plan. Just be sure to bring your test results and a detailed symptom log to your first appointment to make the most of it.
Common Questions We Hear All the Time
Even after you get the hang of reading an allergy test, a few questions always seem to pop up. It's completely normal to have lingering doubts, especially when your own situation doesn't quite match the textbook examples. This is where we clear up the most common points of confusion.
Think of this as your go-to guide for those final "what if" questions. We’ll cover the things we hear most often to help you move forward with confidence.
How Accurate Are These Tests, Really?
This is the big one. Both skin prick tests and IgE blood tests are fantastic tools for identifying sensitization, but it's crucial to remember they aren't perfect.
A skin test, for instance, is excellent for ruling things out. A negative result for an environmental allergen like pollen or pet dander is about 95% accurate. If it's negative, you can be pretty confident that's not your trigger.
But here's the catch: their power to predict a true clinical allergy isn't quite as strong. False positives can and do happen, especially with food allergy panels. Blood tests are generally seen as comparable in accuracy, but neither test can predict how severe a reaction will be. Your personal symptom history is always the most important piece of the puzzle.
Should I Get Retested, and How Often?
Allergies aren't always a life sentence—they can absolutely change over time. This is especially true for children, who often outgrow allergies to common culprits like milk, eggs, and soy. Adults can see their sensitivities shift, too, sometimes developing new ones or finding old ones have faded.
- For food allergies: Retesting every one to two years is common, particularly for kids, to check if they've outgrown an allergy.
- For environmental allergies: These tend to be more stable in adults. However, retesting every few years makes sense if your symptoms change or your current treatment plan just isn't cutting it anymore.
The best approach is always to discuss the timing with your allergist or healthcare provider. They can recommend a schedule that makes sense for your specific situation.
What if My Test Is Negative but I Still Have Symptoms?
This is a frustrating, but surprisingly common, scenario. If your test comes back negative but you're still convinced something is triggering your reactions, a few things could be happening.
A negative test doesn't automatically mean you're in the clear. Your symptoms could be caused by a non-IgE mediated allergy, a sensitivity that standard tests don't pick up, or an allergen that wasn't included in your specific test panel.
For example, you could be reacting to a food additive, experiencing non-allergic rhinitis, or dealing with a different underlying condition altogether. This is precisely when you need to partner with an allergist. They can dig deeper, explore other diagnostic tools, and help you find the true source of your discomfort. Your real-world experience is valid, and a good practitioner will always take it seriously.
At BARB N.P., we believe clear answers are the first step toward feeling your best. Our curated selection of at-home health tests, skincare, and wellness products is chosen to support you on your journey. Explore our collections and find the tools you need to take control of your well-being today.
📌 Visit us at https://barbnp.shop to learn more.


